7. The Wolfson Hospital and further struggle
The construction of a new medical center in the area of Jaffa – Holon – Bat-Yam was planned because of the deterioration of the Donolo Hospital in Jaffa. The old Donolo Hospital, dispersed in several barracks, was rapidly becoming obsolete. As there was no other general hospital nearby, a replacement was urgently needed. In 1963, construction of the new hospital was started in the Tel Giborim section of Holon. However, the “disappearance” of huge sums of money designated for continuation of work, halted the construction. According to the official version, the funds were diverted from the Ministry of Health to the coffers of one of the political parties, an event known as the “Itzhak Rafael affair”. Due to shortage of capital, the construction was delayed for many years and, quite likely, would never have been renewed, were it not for the generous help of the British-Jewish philanthropist, Sir Isaac Wolfson, whose magnanimous contributions enabled the work to continue. The building was completed in the beginning of 1980, and the Edith Wolfson Hospital (named in honor of Sir Wolfson’s wife) opened in Holon at a solemn ceremony on March 4th 1980 (Fig. 48). On April 1st my department was transferred to the new establishment. Because the operating rooms were not quite ready, I used to spend most of the time in my office, reading or writing. On several occasions I operated at the Assaf Harofe Hospital, and in May, I managed to arrange a trip to Marseilles, France, to participate in a convention on pleuroscopy. The orderly work started only in July, with opening of the operating rooms.
Initially, the Wolfson Hospital was planned to replace Donolo and was intended to have two surgical services – the two that functioned in Donolo. Because of the last moment’s decision to convert Shmuel Harofe into a geriatric hospital and the long-lasting deliberations regarding the future of the “acute” services at Shmuel Harofe, my department was not taken into account and, in a way, became superfluous: a third surgical service in the hospital where only two were planned. The hospital administration came to Wolfson from Donolo and did not want us. For them, we were not a transfusion of fresh blood that would rejuvenate and invigorate their aging institution, but invaders who came to rob them of all that by the force of habit became “theirs”. They approached the team of Shmuel Harofe with undisguised hostility. From the first moment we were treated as unwanted “stepchildren”, and we felt it acutely. The 73 beds appropriated to surgery were divided according to the scheme that only the hospital administration could understand. The first surgical service was assigned 30 beds, the second service, 25, and the third (my service), 18. This, despite the fact that in the Donolo Hospital each of the two surgical services commanded only between 25 and 30 beds and performed only general surgery, while my department in Shmuel Harofe had 45 beds, and served both general and thoracic surgery. Also, the first service, since the death of its chief, Dr. Haim Izak, did not have a permanent chief, only an acting chief. This was with complete disregard of the requirements of the Scientific Council concerning accreditation for training residents in surgery. In Israel, for full accreditation, a surgical service must have a minimum of 30 beds, and for partial accreditation (in collaboration with other services) a minimum of 25 beds. The first surgical service that did not have a permanent chief until March 1982 and therefore could not become accredited, was assigned 30 beds, as required for full accreditation. The second service, with its 25 beds, could barely become partially accredited. My service would not qualify even for partial accreditation. My appeals and petitions to the administration fell on deaf ears. I conducted a number of conversations with senior officials in the Ministry of Health, individuals who were personally involved in the transfer of my department and its integration within the Wolfson Hospital, but they ignored my arguments. In case I desired further conversations in the Ministry of Health, they advised me to apply for an audience through my hospital administration, according to the rules. A “useful” suggestion, indeed. I was completely helpless. Throughout all my professional life, I do not remember a period of greater anguish than the first four years at Wolfson. Only in 1985 did the hospital director make the fortunate decision to retire at the age of 62, and in his place came Dr. Amnon Shahar from the Sheba Medical Center. He had not been involved in the Donolo Hospital politics and was not prejudiced against the Shmuel Harofe “invaders”.
Among the surprises that the administration had in store for me, was its unshakable desire to get general surgery out of my department and to limit its activity to thoracic and vascular (!) surgery, this branch that I had stopped practicing several years earlier. I was not sufficiently skilled in it, and I had good reasons to believe that the administration intended to make me fail by imposing it on me, and by forcing on me a “deputy” who would “help me” with vascular surgery and in parallel sabotage my work. An appropriate candidate did, indeed, work in the hospital at that time, and the administration tried to force him into my department against my manifest opposition. The struggle over the character of my department reached the Ministry of Health, but I had a strong legal base to lean on: that famous letter of appointment from 1970, when I won the tender for the position of Chief of the Department of Surgery (Thoracic and General). 22 The law of tenders was on my side and the hospital administration had to retreat.
In parallel, several changes occurred in the hospital. Dr. Alex Dinbar, chief of the second surgical service, also became disenchanted with the Wolfson Hospital atmosphere. He applied for a position of chief of surgery in the Meir Hospital in Kfar Saba, and won. In his place came Dr. Arie Merhav from the Ichilov Hospital. After a year of trial, he returned to Ichilov. Following him, there was one year of interregnum, when Dr. Dona served as acting chief, and in September 1983 Dr. Yehuda Adam arrived from the United States. After three months, in December of the same year, he too decided to leave, and returned to the United States.
This rapid rotation of chiefs paralyzed the work of the second surgical service completely. In 1984 it was decided to “freeze” it, and its beds were divided between the first and the third services. Now I could apply to the Scientific Council. Accreditation of my department for training of residents followed promptly.
Likewise, the hospital directors changed from time to time. Dr. Shahar remained in Wolfson until 1989 and then returned to the Sheba Medical Center. Dr. Waysbort served as acting director from 1989 to 1993, and in 1993 Dr. Moshe Mashiah came, bringing with him stability and progress.
* * *
The affiliation of my department with a medical school was delayed for a number of years. My petitions to the successive deans of the Faculty of Medicine of the Tel Aviv University remained without response for a long time. In 1986 I was invited to Prof. Theodor Wiznitzer’s home. At that time he was not dean anymore – Prof. Haim Boichis had replaced him. While we drank coffee, Wiznitzer told me some details connected with that tender in 1957, when my candidacy for residency in Hadassah had been rejected. Also, in contrast to his earlier indifference, he promised to take an interest and to find out the reasons the medical school was not responding to my repeated petitions for affiliation. His “interest” appeared to be quite effective, because in the beginning of the new academic year, in October 1986, I was appointed to the Faculty of the Tel Aviv University Sackler School of Medicine. I did not have to pass through all the ranks of academic promotion, such as instructor, lecturer and senior lecturer, but was appointed directly as Associate Clinical Professor of Surgery (Fig. 49). Together with the appointment, came a variety of functions, such as lecturing in the Medical School, instructing groups of students in the hospital, and others. During the years that preceded my appointment, I missed students greatly, and now I received them with enthusiasm.
* * *
The job of instructing physicians and turning them into expert surgeons brings both joy and obligations, and sometimes disappointments. During the years, many physicians started their training in my department. Some were good, others very good or excellent. But there were also individuals who did not complete their tour of education. I remember a resident who, while admitting a patient, wrote that normal breath sounds were heard over both lungs. In the past that patient had undergone a left pneumonectomy (total resection of the left lung). Was the resident unable to recognize the absence of breath sounds over the left lung? Did he not see the large operative scar? No. It was a simple case of laziness and cheating. The doctor admitted that he did not examine the patient: “Everybody’s breath sounds are the same anyway, so why bother with examination?” This resident did not stay long in my department. There were also cases of gross meanness. I remember two residents who started working on my service, and without telling me, tried to get residency positions in another hospital. When those positions became available, they left my service without a moment’s notice. I could have tried to hold their paychecks, but what good would that do? They foiled me and failed me, but I learned something from this experience.
It is, therefore, gratifying to recollect those residents who excelled in intelligence and in performance. Their achievements are the true measure of my work as an educator.
I mentioned Dudu Schneider in the preceding chapter. Another striking example was Manoucher Robenpour, a young physician, just out of medical school. He managed to escape from Iran, arrived in Israel and came to me looking for a job. As a newcomer to Israel, he did not know Hebrew. My first impression of this graduate of the Teheran University was not particularly favorable (what can one learn in Teheran?). But he came to me in 1985, several years before the onset of the great immigration wave from the Soviet Union, when we were very short on staff. Discussing his application with Dr. Kaufman, we arrived at a conclusion that the newcomer could not be any good. However, he could assist on operations and participate in emergency night calls. At that time, even construction of the “on call” list was difficult. I had no choice, but to accept him.
Dr. Robenpour had some surprises in store for me. He worked with exceptional diligence. He came to see patients with difficult clinical problems every night, even when not on call, read scientific journals and books pertaining to those problems and stimulated discussions. In addition, he found time to write a number of articles for publication. I learned from Manoucher that it is not important what university one graduates from, but the personality of the graduate. In 1987 I recommended him for citation as an outstanding resident. He stayed in my department for three years, but eventually went into plastic surgery, of which he had always dreamed. At present he is in private practice – a well-known plastic surgeon in Israel.
There was another bright star among my residents. One day in 1993, a young female doctor entered my office, told me of her desire to become a surgeon and asked whether I would accept her for residency training. “Little girl”, I though skeptically, “how will she fit into surgery?” Eventually I accepted her for a trial period, but because of my earlier experience, I exacted a promise from her that she would not simultaneously look for another job. This graduate of the Ben Gurion University School of Medicine, Dr. Yael Refaely, worked hard, had a brilliant mind, excellent clinical judgment and manners, and the skillful hands of a born surgeon. During her work on my service we wrote and published together seven clinical papers. Her most important features were honesty, integrity and courage to carry a responsibility. I remember well an operative complication in which Yael was involved – a bleeding that could have been easily avoided. In other, similar cases, I saw how the physician who caused the complication, tried to shift the responsibility onto others who participated in the operation (“he told me to do so…”). Instead of trying to evade responsibility, Yael entered my office, told me about the case, accepted full responsibility for the complication and asked me whether this was not the time for her to leave surgery and find a different branch of medicine that would fit her better. I took that idea out of her head. From complications such as hers, one should learn, not run away. Only someone who does not operate, has no operative complications.
Among the doctors who worked on my service (both, residents and experts), Dr. Refaely was the only one, the head nurse never yelled at. She was like a flower on the service, until that day when we both left – I went into obligatory retirement; Yael – to continue her residency at the Sheba Medical Center, where she still works, now as a certified specialist in thoracic surgery (Fig. 50).

Fig. 50. “The girl who wanted to be a surgeon” – Dr. Yael Refaely at the time of her work on my service.
* * *
In April 1976 a 53-year-old patient was referred to me because of coughing and raising sputum mixed with blood. He smoked two packs of cigarettes a day for most of his life. His chest roentgenogram disclosed a tumor in the left lung. At the operation I found cancer (squamous cell carcinoma) at the base of the lung. The tumor invaded the diaphragm and the spleen. I resected the lower lobe of the lung along with part of the diaphragm and the spleen, and closed the rent in the diaphragm with a patch of plastic mesh (marlex). The postoperative course was uneventful. The remaining upper lobe of the lung expanded well and filled the chest cavity, and the patient recovered promptly. In spite of my repetitive advice and his wife’s assertive demands, he did not stop smoking and refused to accept any further treatment – either by radiotherapy or by chemotherapy. But the operation apparently had been adequate, the cancer did not recur, and the patient enjoyed another 17 years of good life. He died at the age of 70, from a different kind of cancer (sarcoma) in his other lung. We remained friends until the day of his death, and during those 17 years that he won, I shared many of his joys, such as the weddings of his daughters and the births of his grandchildren. The course of cancer is sometimes a matter of luck, more than anything else.
* * *
Another victory, with a romantic background, occurred when a 24-year-old woman was attacked by her former boyfriend. He grasped her hair with his one hand, and with a knife held in the other, stabbed her eight times in the belly and on both sides of the chest. This event occurred very close to our hospital. There was no time for the usual routine evaluation. Without roentgenograms or any other tests she was brought into the operating room. She had no palpable pulse and her blood pressure was zero, but her heart sounds and breath sounds were still audible. Her bleeding had to be stopped before anything else. I was ready to begin the incision, when the anesthesiologist said: “Dov, you are wasting your time, she is dead”. I started the operation. Inside the abdomen I found two liters of clotted blood. There were several bleeding stab-wounds in the liver that I sutured, a torn spleen which I resected, and several cuts in the intestines and in the stomach – all treated according to needs. By the time of closing the abdomen, her blood pressure rose to 60. The injuries to the chest were taken care of by inserting tube drains on both sides. Over one liter of blood was drained from the chest, but the bleeding diminished gradually, and there was no need to open the chest. The patient recovered. One year later I attended her wedding. When I danced with her, she seemed alive and very much so. I would point this out to the anesthesiologist, but he was not present at the wedding.
* * *
Unfortunately, surgery is not composed only of victories and joys. A short time after the operation just described, I treated a 26-year old man, married and father of two daughters, both under 3 years. He had cancer of a rare kind (adenoid cystic carcinoma) extending from the lower end of the trachea (windpipe), along the entire left main bronchus, down to its bifurcation into two lobes. The patient’s family understood the severity of the situation. I remember his mother’s emotional appeal: “Doctor, gouge my eyes out, but save my child”.
The surgical treatment of this kind of neoplasm involves resection of the entire left lung, a procedure that requires opening the chest on the left side. But because of the extension of the tumor to the trachea, the resection must involve the lower end of the trachea as well, and connecting the trachea to the bronchus of the right lung – the only lung left to the patient. This procedure cannot be performed from the left side, because the aorta obstructs the surgeon’s approach to the trachea (Fig. 51). It was necessary, therefore, to open the chest on both sides – a very traumatic operation. I knew of the exceedingly great danger to the patient, but this kind of cancer was not sensitive to radiotherapy and there was no effective chemotherapy. The only hope was in resection as described, with two operating teams working simultaneously on both sides of the patient.
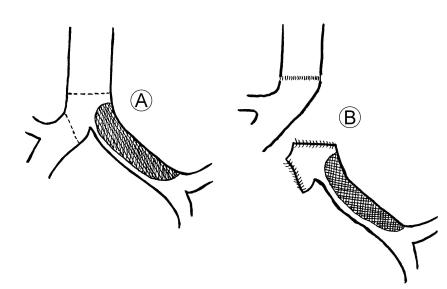
Fig. 51. Schematic drawing of the operative finding and the procedure. A. Criss-crossed area indicates the tumor. Broken lines mark the limits of the resection. B. The left lung had been resected together with the lower part of the trachea and the right bronchial stump. The right bronchus had been sutured to the trachea.
The operation was technically successful, but at the end, the patient was unable to breath spontaneously, and it was impossible to detach him from the artificial respirator. He remained in the operating room, ventilated by the machine until the late evening – the time of his death. It is difficult to describe the conversation with his mother and wife – and I will not try. For me, it was an exceptionally traumatic experience.
* * *
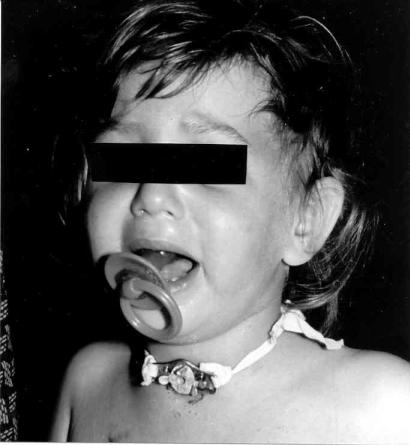
Another tragic case was that of a girl, less than three years old, from a religious agricultural settlement. She played in the yard in front of her house, near her father’s tractor. The father did not notice his daughter, climbed the tractor and went to work. When he heard his daughter’s screams, it was too late. The girl suffered a severe head injury and was hospitalized for a prolonged time. Her breathing ability was temporarily impaired, and she was ventilated artificially for three weeks. The breathing tube inserted into her trachea caused an inflammatory reaction, resulting in a scar with obstruction of the trachea. The obstructed segment had to be resected, and the girl was transferred to my service (Fig. 52). The operation itself and the immediate postoperative course were uneventful, but after several weeks the breathing difficulties recurred. Bronchoscopy disclosed excessive growth of connective tissue (granuloma), with narrowing at the suture line. I removed the granuloma with a forceps, with immediate restoration of normal breathing. After another three-week period, early symptoms of narrowing recurred. One Friday night the breathing difficulties increased. Because of the onset of the Sabbath, the parents decided to postpone the hospital visit until Sunday. That night at dinner, the girl aspirated a small morsel of food into the trachea and the airway became obstructed. Sabbath notwithstanding, the parents took her to the hospital, but she was dead on arrival. Resuscitative measures were ineffective. According to the parents wish, autopsy was not performed. There was no doubt about the cause of death. The parents – deeply religious – accepted theirs daughter’s death as fate and God’s wish.
* * *
Medical negligence is bad. It may cause a patient’s deterioration and death, and must always be avoided. But it is not always the physicians who are at fault. It may be the patient’s own ignorance or plain stupidity that prevents the necessary treatment. An unforgettable case comes to mind, from the times of my surgical residency in New York, 40 years ago. A woman in her early forties visited the outpatient department because of a “wound” in her chest. On examination there was a shocking view of the woman’s chest. The left breast was missing. In its place there was a deep crater, 15 cm in diameter, muscles and other soft tissues destroyed. At the bottom of the wound one could see uncovered ribs. The entire cave was full of pus, dissipating offensive stench. It was an obvious case of an extremely neglected breast cancer. It must have taken years to reach this level of breakdown. To my questioning about presence of a mass in her breast at some earlier time, the patient answered “yes, there had been a mass and it grew over several years. Afterwards the skin ulcerated, and that wound too kept growing.” She added, that she avoided an examination by a physician, because of her worry that it might be cancer, and the doctor would suggest an operation. During all those years she even managed to conceal the horror from her husband. “So why did you come now to the hospital?” “Because last week my husband discovered the wound and forced me to come.” At that time, the management of breast cancer, this advanced, involved resection of both ovaries (oophorectomy) because of their hormonal influence on this neoplasm. This was the first case of oophorectomy in my career.
* * *
The following story illustrates the importance of experience in clinical practice – a feature that does not depend on a high level of education. I remember an incident from my internship in Hadassah, during my rotation on the pediatric service. One night I was called to see an infant. One of the older nurses did not “like” the baby’s breathing. I examined the infant and found nothing wrong, but because I did not have previous experience with little babies, I decided to alert the pediatrician on call. He came, examined the infant, and also did not find anything exceptional. He calmed the nurse, and we both went to sleep. Before dawn the infant died. What happened? We never found out. But it is clear to me that the nurse had extensive clinical experience and knew something about newborn babies. She was right in her impression that something was wrong. The infant was not saved, but my decision to alert the pediatrician was correct. Perhaps he should have alerted a more experienced, senior pediatrician?
* * *
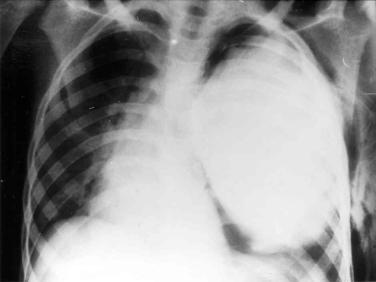
Following is an example of a “medical miracle”. This is a story about an 11-year-old boy with a huge mass inside his chest on the left side (Fig. 53). He was sent to me in 1976 for a possible resection. The tumor was malignant; it invaded the mediastinum and the chest wall (Fig. 54). Resection was impossible. I took a biopsy and closed the chest. Histological examination disclosed neuroblastoma, a malignant tumor of the nervous system in children, with a very bad prognosis. The child was referred to the oncological service for treatment, but his parents procrastinated, and he was not treated. He also never came for a follow-up examination. Several years later, when I reviewed the experience of my department with similar tumors in the lung, I was unable to trace this patient and to find out what had happened to him. I assumed that he must have died. However, 23 years after the operation, a physician from another hospital called me, requesting detailed information about this patient. It turned out that he was hospitalized for a condition not related to his childhood tumor. He did not keep his hospital discharge summary from 1976 and did not know much about his disease, but he remembered my name, which helped his physician to find me. The tumor had vanished without a trace. 23
What is a medical miracle? I use this term to describe a clinical course that is contrary to all expectations and cannot be explained. This phenomenon does exist.
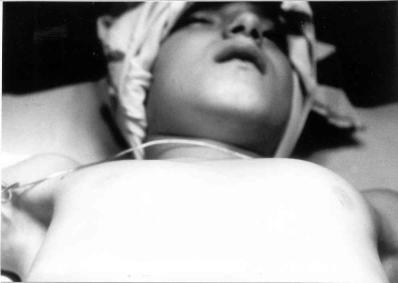
Fig. 54. The patient on the operating table, just before start of the operation. There is a considerable bulge on the left side of the chest, due to tumor invading from within.
* * *
I will conclude this bunch of clinical cases with a story about a patient with Bürger’s disease (occlusion of blood vessels in limbs), a chain-smoker, incurable and without hope. All his limbs were amputated, but his wounds still would not heal because of lack of blood supply. I was involved in his treatment in the Rambam Hospital in 1958. Every week or two we had to amputate a further part of one of his extremities in order to reach a healthier level of tissue, with a chance to heal. His suffering was beyond description. His pain did not react to drugs, including morphine that he received without restriction. His wife was sitting at his bedside, holding a cigarette in his mouth – the cause of his disease, but also his last and only pleasure. No one would stop her from doing it. He told me: “This is not life; I prefer to die, I want to die”. He meant it. It was clear to all that his death was close and no treatment could save or prolong his life; we could only prolong his suffering.
Such patients are not a rarity, today as then. We have no right, legal or moral, to shorten their lives. But do we have the right to prolong their agony?
22 See Chapter 5.
23 A similar case with spontaneous complete disappearance of an invasive neuroblastoma has been described by William A. Nolen in his book “The Making of a Surgeon”, Random House, New York, 1968, p. 201.